Community health providers across Ontario continue to offer steadfast supports to marginalized people

[Using posters like this and sharing messages with partners in the Cornwall region, Seaway Valley CHC staff are supporting their Public Health Unit colleagues who've led the COVID-19 response in the region. Details are below.]
In the last several weeks, as Alliance members across the province have continued and stepped up their efforts to support marginalized people facing the impacts of the pandemic and the effects of measures to slow the spread of COVID-19, we've also seen a lot of centres join Black Creek CHC, Rexdale CHC, Somerset West CHC and other organizations who've led the way on community-led testing and response. We've also seen Alliance members across Ontario jumping in to support the messages and the efforts of their local public health units, and still others taking steps to support increased harm reduction and overdose prevention services to help address the sharp increase in overdose deaths. All over, Alliance members are still working hard every day to support isolated people, deliver food and supplies, as well as checking in people, especially isolated seniors. Here's a review of the some of the stories from different areas:
In the Greater Toronto Area, which has seen some of the fastest rising numbers of COVID-19 cases, Alliance members have stepped up their efforts, with South Riverdale CHC, Unison Health and Community Services joining early leaders on testing and direct COVID-19 outreach and supports at Rexdale CHC, Black Creek CHC, TAIBU CHC, Unison Health and Community Services, and Flemingdon and South Riverdale CHCs. Acting on the knowledge that 1 out of every 4 new COVID-19 cases in Toronto affects a Black family, TAIBU has also partnered with the Scarborough Health Network to launch a COVID-19 helpline to support Black community members with information, guidance and directions to support. In Bramalea, WellFort Community Health Services continues to offer free, community-based testing on site, three times per week in the month of December. All across the GTA, the Anishnawbe Health Toronto's Mobile Healing Team continues to offer accessible testing and other supports to urban Indigenous people in the region, several times per week in different areas. The team was also profiled recently in the Globe and Mail, in an essay by Anishinaabekwe physician Lisa Richardson.
And testing efforts driven by Alliance members and their community partners continue to grow across the province, while adapting to the shifts in the pandemic. In southwestern Ontario, where Windsor-Essex recently entered lockdown, North Lambton CHC continues to offer testing with its partners, including testing for secondary school students in the region. In the Ottawa region, Somerset West, Sandy Hill and Centretown CHCs have all been actively involved in COVID-19 testing, specfically to help reach people not being served by other assessment centres, such as people facing transportation barriers. South-East Ottawa CHC is the lead agency for the Ontario COVID-19 "Supporting High Priority Communities" strategy for Central Ottawa (see image below).
These efforts were highlighted in a big way in late December when the Ontario government released the earlier mentioneded strategy or plan for "Supporting Priority Communities." Alliance members, who in many areas led early efforts (since March) in testing and isolation supports, make up a large proportion of the leadership in these areas, on the chart below. All of these community health organizations have staff who are working directly with their local partners, including public health and hospitals, to ensure:
-Tailored community outreach and engagement, including translation/interpreation, transportion help, and addressing barriers related to health and social inequities-Increased access to testing, including through on-site testing in congregate living spaces, pop-up testing to reach people facing barriers, and mobile testing-Wraparound supports using a case management approach-Increased capacity/locations for isolation facilities, support for short-term case management on site, etc.
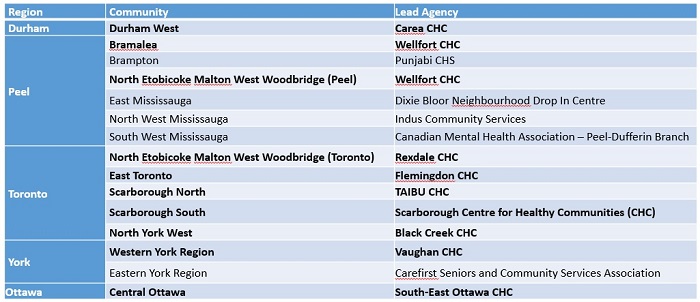
[Alliance members are among those organizations leading the efforts to "support priority communities" -- work they've led for decades, but that has taken on additional importance during the pandemic.]
In Kingston, staff at Kingston CHCs have also been busy helping people get tested for COVID-19 right at their centre, like so many Alliance members across the province, particularly in red and lockdown regions. The centre also pulled together a list of local supports in one spot on their website, to make it easier for people to find the support they need right now. Of course, in other areas of the province, community-based responses have played a key role since last spring, such as with migrant workers being supported by the Delhi Community Family Health Team.
Down the highway in Cornwall, Seaway Valley CHC worked with their community partners to lead a campaign in support of their local public health unit and their efforts to slow spread of COVID-19 and keep people safe. Centre staff felt the health unit deserved support and acknowledgment of their months of hard work so they launched a five-week #AllforPublicHealth campaign. Each Monday a new message goes out on Twitter and Facebook to all of Seaway Valley CHC's partners with a request that they spread the messaging. Here's an example of the campaign's posts, in English and French, passionate calls by Primary Care providers and their partners for us all to support public health, our hospitals, and to help protect marginalized people and those at higher risk due to COVID-19. The centre also helped to lead a flu vaccine campaign that saw some 400 shots per day delivered via a drive-through model, which was a model used in plenty of other places in Ontario, such as this drive led by Niagara Falls CHC.
Advocacy efforts in Toronto paid off as it was announced earlier this week that overdose prevention services would open within shelters, to help reduce the risk of a fatal overdose. Parkdale Queen West CHC's Angela Robertson and South Riverdale CHC's Jason Altenberg led the call, alongside their community partners, to have these services installed. Thanks to both of them and their colleagues for working to making this vital shift a reality that can help save lives this winter and beyond.
Elsewhere, Alliance members continued their ongoing efforts on food security, with examples at Georgian Bay CHC, where an emergency grant from Community Food Centres Canada will help the CHC to reach more people; in Etobicoke, LAMP CHC continues to see increased need, and has stepped up its food security efforts alongside community partners; Carea CHC in Oshawa has teamed with local businesses on a food and toy drive; Access Alliance continued its string of take-away meals for people in need of support; at Centretown CHC in Ottawa, a donation of warm clothing for children is helping out parents in the CHC's Early Years program; in Scarborough, the Scarborough Centre for Healthy Communities is helping to distribute a donation of homemade masks to help keep people safe.
There are literally hundreds of other stories like this, efforts by community health organizations to meet the evolving needs of the people they serve, and across their communities.
If you're reading this and you're from a centre and have a story to share, please email me directly, so I can include yours in my next update: jason.rehel@allianceon.org.







