
The Alliance and its members are uniquely successful, not only in comparison to others in Ontario, but also in Canada and Internationally, as being the largest, most deeply rooted, most successful learning health system that I’ve ever seen.
– Dr. Merrick Zwarenstein, Professor in the Centre for Studies in Family Medicine and Department of Epidemiology & Biostatistics at Western University
In 2015, the Alliance began a journey towards becoming a learning health system. This journey passed a major milestone in October 2020, when our LHS was formally adopted by the Executive Leaders’ Network. Thus our learning health system, EPIC – which stands for Equity, Performance, Improvement, and Change – was born.
All learning health systems follow a similar learning cycle: relevant data is assembled and analyzed; results are interpreted and delivered with tailored feedback; and action is taken to change or improve practice. This generates new data, and the cycle continues. Despite these common elements, every LHS is unique. What is unique about Alliance member organizations will also be unique to the LHS we are building together: it is grounded in our common commitment to health equity and the principles and attributes of the Model of Health and Wellbeing.
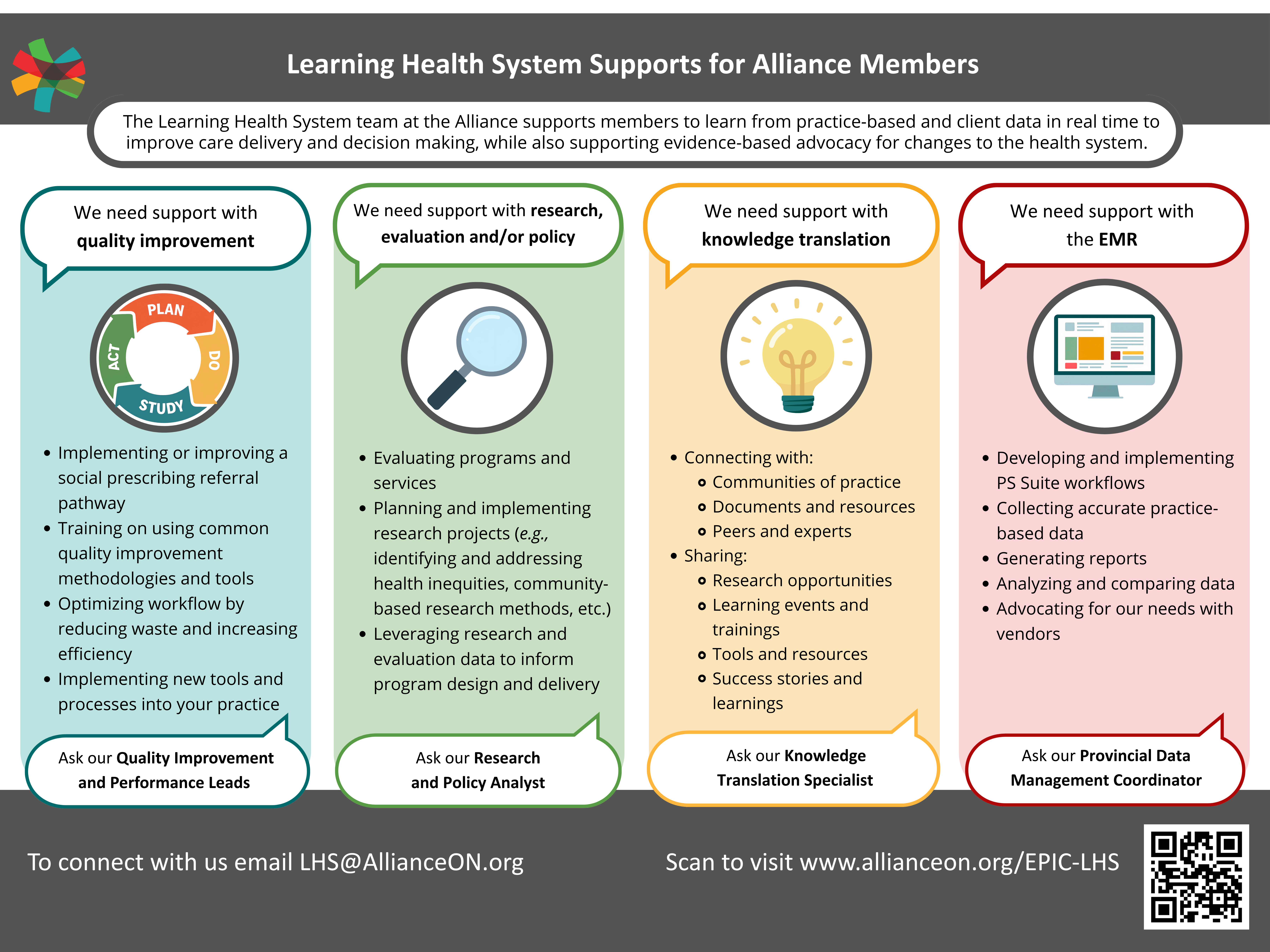
# The EPIC Learning Health system brings together many different Alliance programs and projects, including:
- Research
- Information Management
- Social Prescribing
- Tailored Data Reports
-
Coach-Supported Learning
- Learning Collaboratives
- Rapid Action & Learning Intensives (RALI)
- Tailored Quality Improvement (QI) Coaching
- Peer-Supported Learning
- Learning Events
We communicate about EPIC activities and research through our Alliance eBulletin, EPIC News, and our Research Library.
What is a learning health system?

A Learning Health System (LHS) is characterized by continuous learning and growth. It brings together information from practice and research and feeds it back to teams in ways that are meaningful and useable to them. This in turn leads to practice change that improves care. The participants in a learning health system collect, share, and use information in real time to guide care and improve decision-making. This cycle of continuous improvement results in better client experiences; better health and wellbeing for individuals, communities, and populations; more satisfaction and joy in work for health care teams; and a more effective and sustainable health system. Around the world, this approach to learning and improvement has been increasingly recognized as a key enabler of better health care.
Our Commitment: Responsible Collection and Use of Data
A key aspect of our Learning Health System is a commitment to ensure that data shared is meaningful and actionable. Through our common electronic medical records system (EMR) and our Business Intelligence Reporting Tool (BIRT), we compile and presenting practice-based data in accessible ways that Alliance members can use do drive local improvements and demonstrate their impact.
In addition to supporting local and sector-wide improvement, Alliance data is securely shared with research partners such as ICES and CIHI. This enables it to be included in provincial primary care datasets and to be linked to health system administrative data, both of which help demonstrate our sector's value to the health system.
We are committed to collecting, sharing, and using data in ways that are culturally safe and advance health equity. We work with Black and Indigenous health leaders to ensure we are adhering to principles of data sovereignty, including the EGAP (Engagement Governance, Access and Protection) and OCAP (Ownership, Control, Access and Possession) frameworks.
Strategic Guidance: The EPIC Learning Health System Steering Committee
The EPIC Learning Health System Steering Committee (also known as the EPIC Committee) is a member-led committee consisting of executive leaders, quality managers, and board directors of Alliance member organizations. The Alliance’s Research and Policy team, directed by Dr. Jennifer Rayner, provides backbone support and information to the EPIC Committee.
Drawing from the Model of Health and Wellbeing and our Evaluation Framework, the EPIC committee develops strategies, questions, and indicators for measuring the effectiveness of the LHS. EPIC also informs the development of tailored reports and provides high-level guidance for quality improvement support.
